How cortisol and GR sensitivity often determine your health (from inflammation and cancer to neurological conditions and anxiety).
Stress is a reflection of the body’s entire physiological state and its evolutionary survival mechanisms, largely orchestrated and modulated by cortisol.
Cortisol is the primary “stress hormone” released by the adrenal glands in response to signals from the hypothalamus-pituitary-adrenal (HPA) axis. Its job is to mobilise energy (increasing blood sugar), modulate inflammation, and help the body adapt to short-term challenges (the “fight-or-flight” response). Cortisol is released in response to any increase in demand on the body (real or perceived threats to homeostasis), not just from mental workload.
Glucocorticoid receptors (GRs) are proteins inside cells (especially immune cells, liver, fat, and brain) that cortisol binds to, acting as master regulators that turn genes on and off. Their main purpose is to maintain homeostasis by regulating metabolism, immune function, stress response, and development.
Essentially, cortisol signals that you are stressed, and GRs increase or decrease gene activity to deal with said stress. In other words, when you are out of balance, cortisol is released to restore it. The more GRs are activated, the less sensitive they become; the less they are activated, the more sensitive they are.
How high GR sensitivity leads to shorter stress responses.
Stress has a built-in mechanism, called a negative feedback loop, that is designed to inhibit itself. Cortisol inhibits the release of corticotropin-releasing hormone (CRH) and adrenocorticotropic hormone (ACTH) from the hypothalamus and pituitary gland, thereby shutting down the signal for its own production once a stressor has passed.
This mechanism is largely determined by GRs, with high sensitivity leading to a quicker shutdown of stress and low sensitivity causing stress to continue on and on.
| The effects of GR sensitivity balance | |
| High sensitivity | Low sensitivity |
| Stronger anti-inflammatory effects | Increased inflammation |
| More efficient HPA axis shut-off | Less efficient HPA axis shut-off |
| Lower baseline cortisol production | Higher baseline cortisol production |
| Improved metabolic efficiency | Decreased metabolic efficiency |
| Decreased sympathetic outflow | Increased sympathetic outflow |
The biggest cause of chronic stress and low GR sensitivity is regular stress.
Stress causes more stress. What I mean is that the more stress you have, the worse your stress response gets because your GR sensitivity decreases, lowering the threshold for activation and making it last longer.
Thus, if you want to feel stressed less easily and for less time, you need to reduce the amount of stress in your life. Any decrease in stress breaks the negative spiral of declining GR sensitivity, which is key to lasting improvements.
How negative reactions to stress worsen the stress response.
Not only does stress lead to a worse stress response, but your response to stress also often leads to a worse stress response. Thinking negatively is key here. It perpetuates the perception of threat or failure, keeping the body’s stress response systems (the HPA axis) activated even after the stressor has ceased. You need to have a plan for when times are difficult. The quicker you go from stressed to not stressed, the better it will be for you. This could include socialising, hobbies, chores, really, the key is to be focused outwards rather than inwards. This works because thinking less decreases the threat signal.
How to decrease the threat signal.
The stress response also turns off because the neural threat signal that initiated it ceases. Techniques such as cognitive reappraisal (what you think), behavioural coping (resolving or avoiding) and habituation (regular exposure) strongly influence this.
Once the threat is assessed as gone (by sensory input and cognitive appraisal), the prefrontal cortex sends inhibitory signals to the amygdala. This dampens the fear/alarm signal at its source. The hippocampus (critical for memory and context) is densely packed with cortisol receptors. It acts as a major brake on the HPA axis. By providing contextual memory (“this situation looks scary, but was safe last time”), it helps regulate the response.
Low GR sensitivity as a cause of disease and symptoms.
Under normal conditions, cortisol binds to GRs. This activates anti-inflammatory and immunosuppressive pathways, helping to terminate the immune response.
In chronic stress, this system malfunctions:
- Chronic HPA-axis activation: Persistent stress leads to sustained high cortisol.
- GR downregulation/desensitisation: Cells reduce the number or function of GRs to protect themselves from constant cortisol signalling. Cortisol is catabolic and immunosuppressive; constant high levels would be detrimental to long-term cell survival and function. GR downregulation allows for short-term benefit over long-term cost (increased immune defence now, excessive inflammation later).
- Result: Immune cells become less responsive to cortisol’s “stop” signal. The inflammatory response, which should be tightly controlled, becomes dysregulated and prolonged.
This leads to a state of chronic, low-grade systemic inflammation. Your genetics and life experiences then determine which disease state emerges. If you have a genetic defect in organ function, it could lead to chronic inflammatory disease; if you have a genetic defect in growth or apoptosis control, it could lead to cancer. The same applies to any disease state and the various genes associated with it.
Ultimately, stress causes disease and disease causes stress.
Disease and infections as a cause of low GR sensitivity.
The link between infections (such as a virus) and decreased GR sensitivity is robust and supported by decades of research across various pathogens. Infections can disrupt the critical negative feedback loop of the HPA axis through the ongoing inflammation they cause.
Viruses produce proteins or manipulate host cell machinery to directly block GR function. They also trigger powerful innate immune responses, and some of these pathways directly cross-talk with and inhibit GR signalling. Viruses have this effect because it is a highly effective strategy that serves several key purposes for a virus’s “life cycle”. Essentially, with low GR sensitivity, the virus survives longer, which is its aim.
With decreased GR sensitivity, viruses cause prolonged symptoms. You see this with the persistent, low-grade inflammation seen in Long COVID patients with neuropsychiatric symptoms and other systemic conditions. These symptoms are driven by a failure of cortisol to regulate the immune response properly. It leads to a triad of neuroinflammation, neurotransmitter imbalance, and HPA axis dysfunction, which is a validated biological substrate for major depressive disorder, anxiety, fatigue, and “brain fog” seen in post-infection syndromes like Long COVID and ME/CFS.
Future treatments will likely need to address both the pathogen and the host’s dysregulated immune response, including GR sensitivity. Intervening during the acute phase (early stages) to prevent GR desensitisation might be more effective than trying to reverse it years later in a chronic disease state.
Low GR sensitivity as a cause of mental health conditions.
It is often thought by the ignorant that mental health problems are some sort of weakness of the mind. That you need to be stronger and need to simply ‘snap out’ of it. This couldn’t be further from the truth for many.
Low GR sensitivity, through whatever means, whether that is illness, chronic stress or from medication, leads to a failed negative feedback. This leads to chronically high cortisol and sympathetic outflow, hippocampal atrophy, PFC impairment and amygdala hyperactivity. No amount of mental strength will overcome this. Of course, not everyone develops anxiety and depression, though.
It doesn’t affect everyone equally because a combination of genetic, developmental, psychological, and environmental factors creates differential susceptibility or resilience. Essentially, living more enjoyable and rewarding lives, for some, protects them from mental health problems.
STUCK: Low GR sensitivity causes symptoms that further lower GR sensitivity.
Conditions linked to low GR sensitivity (e.g., major depression, PTSD, chronic fatigue) are characterised by symptoms like anhedonia, fatigue, social withdrawal, poor sleep, and unhealthy stress coping behaviours. These behaviours and states are themselves potent physiological stressors.
So much of what someone once enjoyed when they were healthy now causes problems for them when they are unhealthy. Many foods that bring great pleasure are off-limits to many because they cause adverse reactions. Being outside worsens symptoms for some, whether it’s due to light sensitivity, movement or standing, or the anxiety of being in a social setting or away from home. Really, there are so many negative ways illness and mental health problems cause or worsen symptoms that decrease the joy in one’s life.
In an effort to avoid more suffering, illness sort of has this effect, where it leads to safety behaviour, to limit further suffering. This behaviour, though, only accelerates the decline in health because it limits the enjoyment of living, a stressor in itself.
In such situations, you have to treat both the underlying condition and the symptoms to resolve it. If you had an infection that caused inflammation, and now you live an unsatisfying life, you must treat the inflammation and, at the same time, look for alternative ways to enjoy yourself.
Getting worse before you get better.
When treating high cortisol with low GR sensitivity, you have a problem. If you increase GR sensitivity, the high cortisol will remain for some time. Now you will have increased cortisol and increased sensitivity to it (due to high GR sensitivity), and your symptoms will get worse.
With antidepressants, you often see an initial increase in GR sensitivity and cortisol during early SSRI treatment, which is believed to be a primary biological driver of the early activation syndrome that leads to premature discontinuation and early perceived treatment failure (due to increased anxiety, agitation and insomnia).
Supplements have similar challenges. For this reason, it is often recommended to start with a low dose and slowly increase it. Higher doses too quickly often lead to setbacks. Small, meaningful improvements are often the quickest route to lasting results. Lifestyle changes work well because many of them decrease cortisol, thereby increasing GR sensitivity.
Treatment should never be simply medication alone; it should always involve lifestyle changes and emotional support to avoid adverse effects. The support of a good friend often buffers the increased stress.
How to treat low GR sensitivity and resolve the negative cycle.
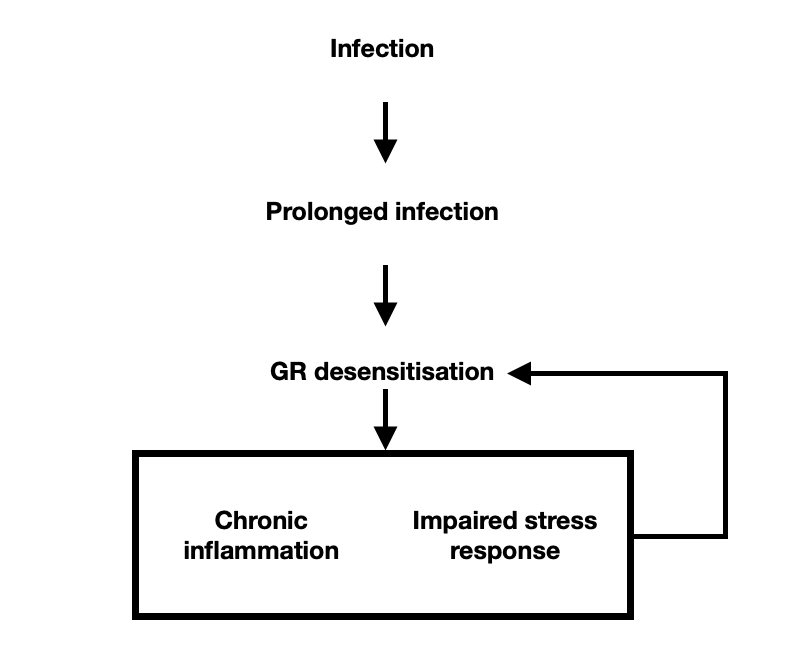
For many, decreased GR sensitivity starts with a prolonged infection, illness or chronic stress. What leads their health to continue to decline is not this infection, illness, or stress, but the decline in GR sensitivity and the reinforcing effects it has on the negative cycle. See below how this works.
Even if you resolve the infection, the cycle continues. The longer the cycle continues, the more difficult it is to treat because fewer and fewer treatment options become available. Chronic systemic inflammation causes imbalances in gut bacteria, increased gut permeability, immune cell dysfunction, insulin resistance, and endothelial damage (the inner lining of blood vessels), all of which further increase inflammation and limit treatment due to heightened sensitivity and vulnerability. Treatments that may have worked in the past now make things worse.
Aspirin further damages the intestinal barrier, increasing its permeability. Antibiotics worsen dysbiosis and potentially allow pathogenic bacteria to flourish. Probiotics, which provide beneficial bacteria to the gut, fail to adhere to the gut lining because harmful bacteria prevent their recolonisation. Fibres intended to feed good bacteria, fuel bad bacteria’s growth and survival, worsening symptoms. Many supplements and so-called health foods have strong antioxidants, vasodilatory and insulin effects, which add to the demands of an already highly stressed body, a demand the body struggles to meet. You become stuck. Treatment only contributes to the problem.
Instead, the focus should be on lifestyle changes and targeted medications.
| How to rebalance GR sensitivity | |
| Increases GR sensitivity | Decreases GR sensitivity |
| Anti-inflammatory foods | Inflammation |
| Light exposure in the morning | Daytime darkness |
| Sun exposure (UVR) | Lack of sunlight (due to vitamin D) |
| Strong social bonds | Social isolation |
| Regular sleep schedule | Sleep loss |
| A positive outlook | A negative outlook |
| Antidepressants | Stimulants (caffeine, nicotine, etc) |
| Environment enrichment | Discomfort |
| Sense of control | High or low calorie diets |
| Mindfulness | Blood sugar imbalances (high/low) |
Enjoyed this article? Then you should read The Health Diary now.
What you have just read is from the chapter on stress in our new book, The Health Diary.
The book isn’t about me, it’s about you. It is strictly content, unlike anything you have ever seen. Much of the information in the book is not readily available online.
If you want new ideas that will change your life, then you want to buy this book.
To get more details on the book, click here.
To buy the book on Amazon, click here.
Medical disclaimer:
The statements made are not intended to diagnose, treat, cure, or prevent any condition or disease. Always consult with your own physician or healthcare specialist regarding the suggestions and recommendations.